Parkinson’s Disease
Parkinson’s disease, a progressive disorder impacting the nervous system, gradually affects various parts of the body controlled by nerves. It primarily impacts neurons responsible for dopamine production within the substantia nigra, a specific region of the brain. The onset of symptoms is gradual, often commencing with subtle indications. Initially, a barely noticeable tremor may manifest in one hand, although stiffness and a reduction in movement speed are also common.
In the early stages of Parkinson’s, facial expressions may become limited, displaying little or no emotion. Walking may exhibit a lack of arm swinging, and speech may undergo changes such as softness or slurring. As the condition progresses, these symptoms intensify, presenting challenges in daily life.
Although widely recognized for its impact on muscle control, balance, and movement, this condition extends its reach to affect various aspects of one’s senses, cognitive abilities, mental health, and beyond.
While Parkinson’s disease currently lacks a cure, there are medications that can significantly alleviate symptoms. Medical interventions focus on improving the quality of life for individuals affected by Parkinson’s. In some cases, surgical options may be recommended by healthcare providers to target specific regions of the brain, aiming to regulate and improve symptoms.
Signs and Symptoms

Motor Symptoms
Non-Motor Symptoms

Understanding these symptoms is crucial for early diagnosis and the development of tailored treatment plans. If you or a loved one is experiencing any of these signs, seeking medical advice promptly is recommended.
Causes and Risk Factors
The exact cause of Parkinson’s remains elusive, but a confluence of factors is believed to contribute to it:

Genetic Influences
Researchers have pinpointed specific genetic changes that can act as catalysts for the disease. While these changes are uncommon, instances where multiple family members are affected by Parkinson’s highlight their relevance. It’s essential to note that these occurrences are relatively rare, emphasizing the complexity of the genetic contribution to Parkinson’s.
Environmental Triggers
Environmental factors, including exposure to toxins, emerge as potential contributors to the risk of developing Parkinson’s disease. Although the risk associated with these triggers is modest, it underscores the complexity of the interplay between genetics and the environment.
Age
The age factor emerges as the foremost contributor to the onset of Parkinson’s disease. Statistics reveal that approximately one percent of individuals aged 60 and above find themselves grappling with this neurological disorder. As the years advance, the risk of Parkinson’s disease becomes more pronounced.
Gender
Parkinson’s disease exhibits a higher prevalence in men compared to women. The reasons behind this gender disparity are still a subject of ongoing research, emphasizing the complex interplay of biological and environmental factors in the development of Parkinson’s disease.

Stages of Parkinson’s Disease
Hoehn and Yahr Staging System
The trajectory of Parkinson’s disease unfolds over years, and its impact can extend over decades. In 1967, Margaret Hoehn and Melvin Yahr introduced a staging system to categorize the progression of Parkinson’s disease.
Stage 1
In the initial stage of Parkinson’s disease, symptoms emerge in a mild form that might go unnoticed. These subtle signs, often missed by the affected individual, are detectable by observant family and friends. Changes in posture, gait, or facial expressions become apparent, with tremors and movement difficulties typically confined to one side of the body. Medications prescribed during this stage prove effective in minimizing these early symptoms, preserving daily functionality.
Stage 2
As Parkinson’s progresses to stage 2, symptoms become more pronounced, making them noticeable to both the affected individual and their close circles. Stiffness, tremors, and changes in facial expressions become more evident, while muscle stiffness may extend task durations. Despite these challenges, balance remains intact. Walking difficulties may arise, and posture alterations become more noticeable. Individuals at this stage can often still live independently, though certain tasks may require more time.
Stage 3
Moving into stage 3 marks a significant turning point in the Parkinson’s journey. While many symptoms mirror those of stage 2, the introduction of balance loss and decreased reflexes becomes more prevalent. Overall movements slow down, leading to an increased risk of falls. Although daily tasks are significantly affected, individuals can still accomplish them with the aid of medication and occupational therapy.
Stage 4
Independence becomes a focal point in stage 4 as individuals can stand without assistance, yet mobility may necessitate a walker or other assistive devices. Living alone becomes challenging due to substantial decreases in movement and reaction times. Daily tasks may become impossible without assistance, highlighting the importance of a supportive environment.
Stage 5
Stage 5 represents the apex of Parkinson’s disease progression, where advanced stiffness in the legs leads to freezing upon standing. Wheelchairs become essential, and standing without assistance becomes nearly impossible. Around-the-clock support is imperative to prevent falls. Additionally, cognitive challenges, hallucinations, and delusions may affect up to 50% of individuals in stages 4 and 5, underlining the multifaceted nature of the disease.

Movement Disorder Society-Unified Parkinson’s Disease Rating Scale (MDS-UPDRS)
Beyond motor symptoms, nonmotor symptoms play a crucial role in understanding Parkinson’s progression. Cognitive changes, mood disorders, sleep disturbances, fatigue, and various other nonmotor symptoms can significantly impact an individual’s well-being. The Movement Disorder Society-Unified Parkinson’s Disease Rating Scale, encompassing both motor and nonmotor aspects, provides a comprehensive evaluation, recognizing the intricate nature of the disease beyond its visible symptoms.
Diagnosis and Early Detection
Unraveling the complexities of Parkinson’s disease begins with accurate diagnosis and early detection. Understanding the process is crucial for timely intervention and improved management. Let’s delve into the intricacies of how Parkinson’s disease is diagnosed, shedding light on essential aspects that guide healthcare professionals.
Clinical Evaluation:
The journey to a Parkinson’s diagnosis often commences with a thorough clinical evaluation. This involves a detailed examination of medical history, symptom manifestation, and a comprehensive neurological assessment. Skilled healthcare professionals analyze motor symptoms, observe movement patterns, and assess factors such as tremors, stiffness, and balance issues.

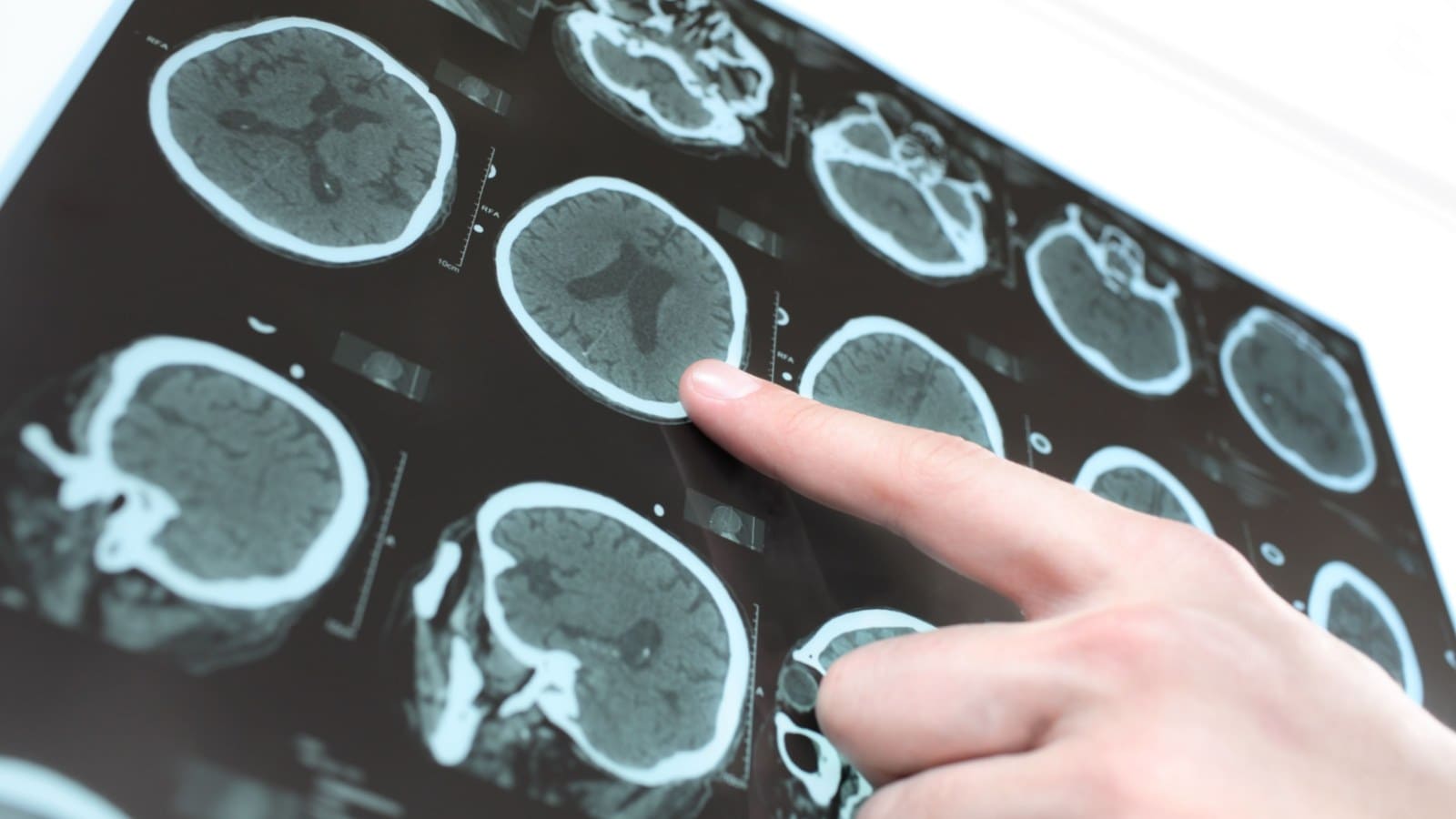
Specialized Testing
While clinical evaluation forms the foundation, specialized testing plays a pivotal role in confirming a Parkinson’s diagnosis. These tests may include DaTscan imaging, which examines dopamine levels in the brain, and blood tests to rule out other conditions with similar symptoms. Additionally, neuroimaging techniques like MRI and CT scans may be employed to provide a detailed view of the brain’s structure.
Diagnostic Criteria
The diagnostic journey adheres to established criteria, such as those outlined by the Movement Disorder Society (MDS). These criteria help guide healthcare professionals in accurately identifying Parkinson’s disease and differentiating it from other neurological disorders.
Importance of Early Detection
Early detection is paramount in managing Parkinson’s disease effectively. Detecting the condition in its early stages allows for timely intervention, symptom management, and the implementation of strategies to enhance overall quality of life. It empowers individuals and their healthcare teams to proactively address challenges, providing a foundation for a more informed and comprehensive approach to care.
Treatment Options
Effectively managing Parkinson’s disease involves a multifaceted approach, encompassing various treatment options tailored to address the unique needs of each individual. Let’s explore the diverse strategies employed in the treatment landscape, focusing on enhancing symptom control, improving quality of life, and fostering individualized care.
Medications
Medications play a central role in alleviating the symptoms of Parkinson’s disease. Levodopa, a precursor to dopamine, is a key component, effectively addressing motor symptoms. Other medications, such as dopamine agonists, MAO-B inhibitors, and anticholinergics, may be prescribed to complement the overall treatment plan. Fine-tuning the medication regimen is a dynamic process, often requiring adjustments to achieve optimal symptom management.
Physical Therapy
Physical therapy emerges as a vital component in Parkinson’s management, aiming to enhance mobility, flexibility, and overall physical function. Specially tailored exercises and rehabilitation programs, conducted under the guidance of experienced therapists, contribute to improved motor skills and help individuals navigate daily tasks more effectively.
Deep Brain Stimulation (DBS)
In advanced stages, Deep Brain Stimulation (DBS) offers a surgical intervention to manage motor symptoms. This procedure involves implanting electrodes into specific areas of the brain, regulating abnormal impulses and mitigating symptoms. DBS is considered when medications alone are insufficient in controlling motor fluctuations.
Speech and Occupational Therapy
Parkinson’s disease can impact speech and daily activities. Speech therapy addresses communication challenges, helping individuals maintain and enhance their verbal expression. Occupational therapy focuses on adapting daily tasks, improving fine motor skills, and fostering independence in daily living.

Lifestyle Modifications
Embracing lifestyle modifications can significantly contribute to Parkinson’s management. Regular exercise, a balanced diet, and adequate sleep play pivotal roles in overall well-being. Individuals are encouraged to adopt a holistic approach to their lifestyle, considering factors that positively impact both physical and mental health.
Supportive Care
Supportive care, including counseling and support groups, offers emotional and psychological assistance to individuals and their caregivers. Navigating Parkinson’s disease involves not only physical but also emotional resilience. Supportive care initiatives foster a sense of community, providing avenues for shared experiences and coping strategies.
