Multiple Sclerosis
Multiple sclerosis (MS) is a chronic, autoimmune, and often disabling neurological disorder that affects the central nervous system (CNS), which includes the brain and spinal cord. In MS, the immune system mistakenly attacks the protective covering of nerve fibers called myelin, leading to inflammation and damage. This disrupts the normal flow of electrical impulses along the nerves.
Types of Multiple Sclerosis
Multiple Sclerosis (MS) manifests in different forms, each with its unique characteristics. Here are the most common types of MS:

Common Symptoms of Multiple Sclerosis
Early identification of MS symptoms is paramount for timely intervention. Common manifestations include:

Distinct Physical Symptoms
Vision and Sensory Disturbances


Neurological and Cognitive Afflictions
Emotional and Mood Disturbances
When to See a Doctor
The diverse symptoms associated with Multiple Sclerosis (MS) may be indicative of various conditions, making it crucial to seek medical advice when experiencing unexplained symptoms. Knowing when to consult a doctor is paramount for timely intervention and appropriate care.
Seeking Medical Guidance: Key Indicators

GP Consultation and Beyond
Understanding the urgency of seeking medical attention when symptoms arise is pivotal for early detection and effective management of Multiple Sclerosis. If you find yourself experiencing unexplained symptoms, do not hesitate to consult with a healthcare professional for timely evaluation and guidance.
Diagnosing Multiple Sclerosis
The journey to diagnosing Multiple Sclerosis (MS) is multifaceted, varying in speed for different individuals. A comprehensive examination is central to the diagnostic process, incorporating several crucial components to ensure accuracy and efficiency.

Elements of a Comprehensive Diagnosis
International Standards: The McDonald Criteria
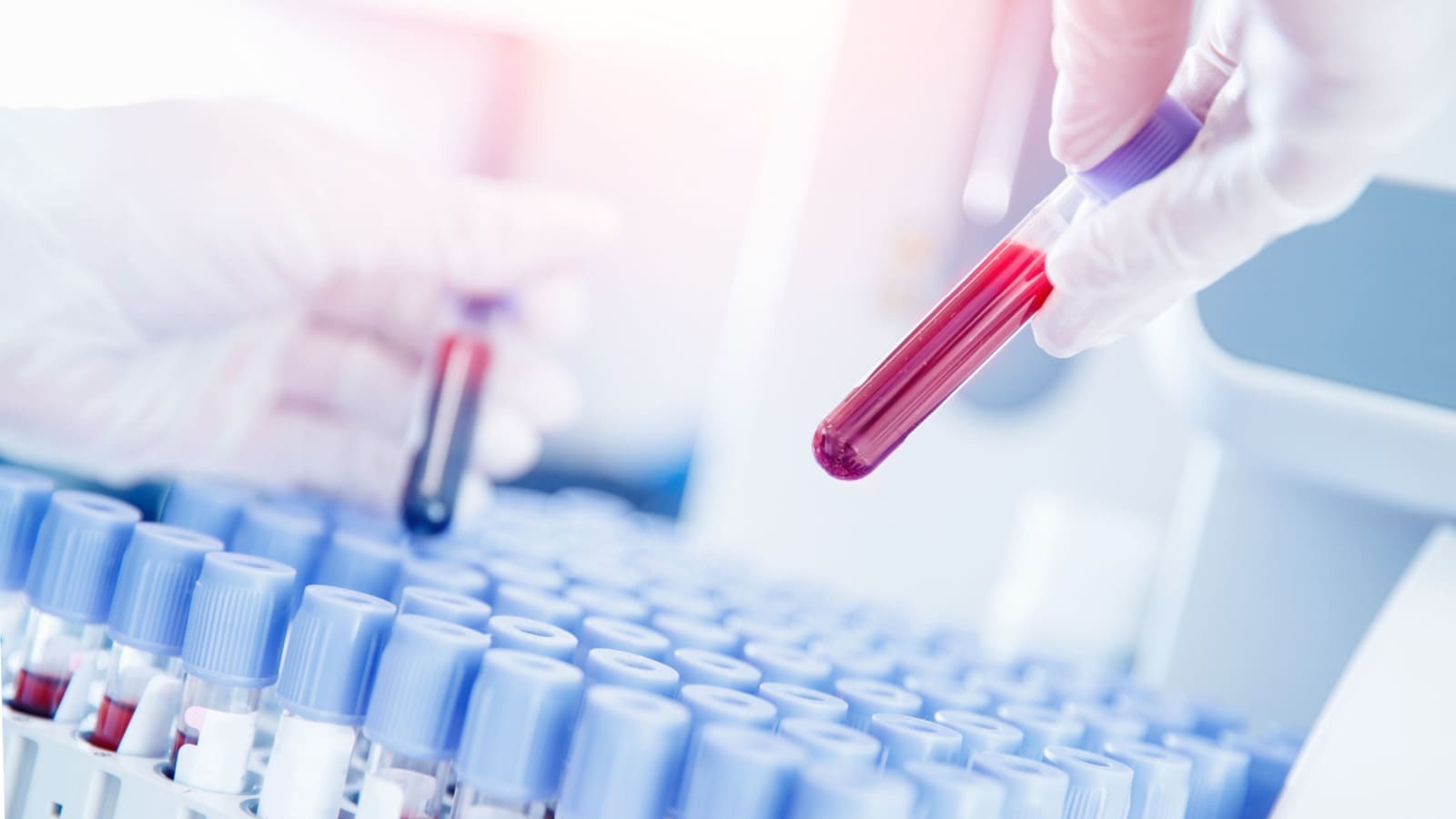
Supplementary Diagnostic Measures
Understanding the complexity of MS diagnosis underscores the importance of a multidimensional approach. By integrating clinical examinations, advanced imaging, adherence to international guidelines, and supplementary tests, healthcare professionals ensure a thorough and accurate diagnosis, paving the way for targeted and effective management strategies.

Treatment Options
In the realm of Multiple Sclerosis (MS), while a definitive cure remains elusive, there exists a spectrum of treatments aimed at managing the condition and alleviating its symptoms.
Tailoring the approach to your unique set of symptoms and challenges, the treatment strategy may encompass various interventions:
It’s essential to note that, regrettably, as of now, there is no specific treatment capable of impeding the advancement of inactive progressive MS, devoid of relapses or MRI activity. However, ongoing research endeavors are actively exploring a multitude of therapies with the potential to address this specific aspect of the condition.
In navigating the landscape of MS treatments, the focus remains on refining existing approaches and discovering novel interventions that hold promise in enhancing the quality of life for individuals affected by this complex neurological disorder.
Living with Multiple Sclerosis
Coping Strategies for Multiple Sclerosis
Living with MS necessitates adopting coping strategies to navigate daily challenges. Psychological support, stress management, and resilience-building techniques empower individuals to face the complexities of the condition with strength and fortitude.
Building a Support Network
A robust support network is instrumental in the MS journey. Connecting with others facing similar challenges, whether through local groups or online communities, provides emotional support and valuable insights, fostering a sense of camaraderie.

